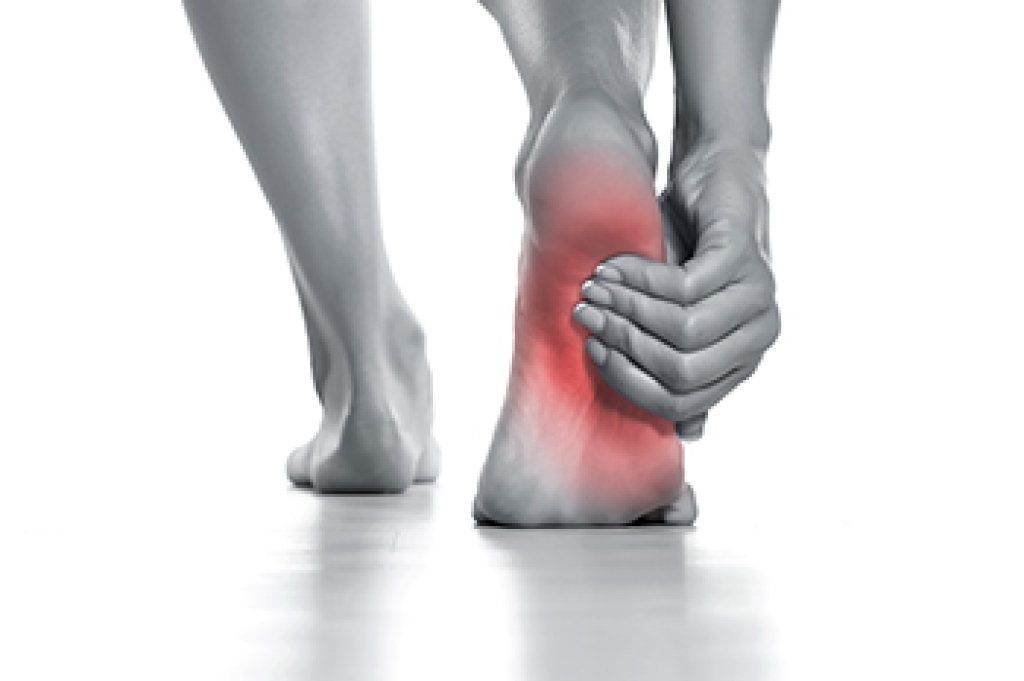
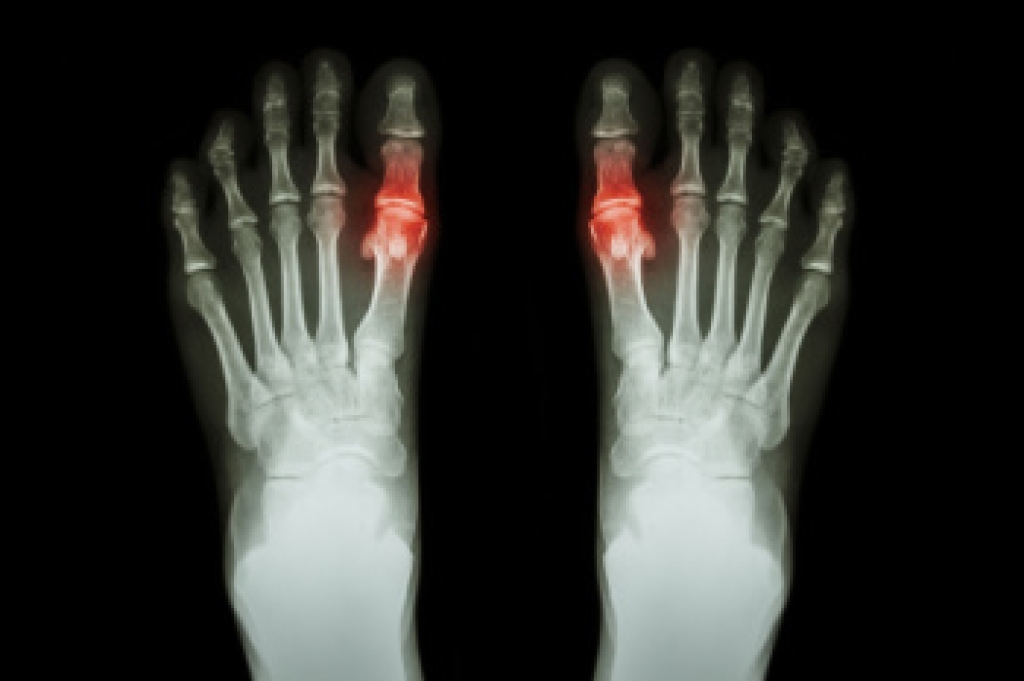
Balance issues often begin with problems in the feet and ankles, especially as people age. Good balance depends on being able to feel the ground and move with stability. Diabetes-related nerve damage, called neuropathy, can reduce feeling in the feet and affect the balance. Fallen arches, arthritis, joint stiffness, and painful foot deformities can also change the way a person walks and increase the risk of falling. Shoes that do not fit well or do not provide enough support can further affect balance and lead to slips or trips. A podiatrist can examine foot structure, check circulation and nerve function, and identify problems that affect balance and safe movement. Treatment includes custom orthotics, bracing, and guidance on supportive footwear. Improving foot stability can help retain balance and reduce the risk of falls. If you have injured your foot or ankle from falling, it is suggested that you schedule an appointment with a podiatrist for effective treatment solutions and prevention tips.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with one of our podiatrists from Comprehensive Footcare Clinic - Hawaii. Our doctors will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Honolulu, HI . We offer the newest diagnostic and treatment technologies for all your foot care needs.